Pain Management During Labor & Delivery | Tips & Tricks To Manage The Labor Pain | NextMamas.

Pain during labor is considered similar in degree to that caused by complex regional pain syndromes or the amputation of a finger. The pain is not life-threatening in healthy women; however, if not managed appropriately, it may result in worse postnatal depression. Furthermore, pain during labor has been associated with post-traumatic stress disorder and impaired cognitive function.
During labor, a stress response is initiated that can result in the release of corticotropin, cortisol, norepinephrine, beta-endorphins, and epinephrine. Epinephrine can lead to prolonged labor through its relaxant effect on the uterus.1 Additionally, maternal cardiac output, systemic vascular resistance, and oxygen consumption are increased.
Not all women experience the same level of pain during childbirth. This variability is attributed to a number of factors—primarily nulliparity and the use of IV oxytocin, both of which are associated with more intense labor pain. Other factors contributing to increased pain during labor include younger maternal age, lower back pain during menstruation, and higher maternal or fetal weight. Women who have attended childbirth classes and those who have performed aerobic- conditioning exercises during the pregnancy may experience less-intense labor pain.
Pain Management
To manage labor pain effectively, it is useful to understand its origin through the different stages of labor. In the first stage of labor, the pain—resulting from both rhythmic uterine contractions and progressive cervical dilation—is transmitted through the visceral afferent nerves to the spinal cord via segments T10–L1. The patient typically reports pain over the lower abdomen, and in many cases the lower back and sacrum. As labor progresses, the perineum stretches and transmits signals through the pudendal nerve and sacral nerves S2–S4. This stage is shorter than the first stage, but the pain—principally somatic—is more intense.
A number of options are available for pain management during labor, including regional (or neuraxial) anesthesia, systemic opioid analgesia, continuous labor support, pudendal blocks, immersion in water during the first stage of labor, sterile water injections in the lumbosacral spine, hypnosis, and acupuncture.
Epidural Anesthesia
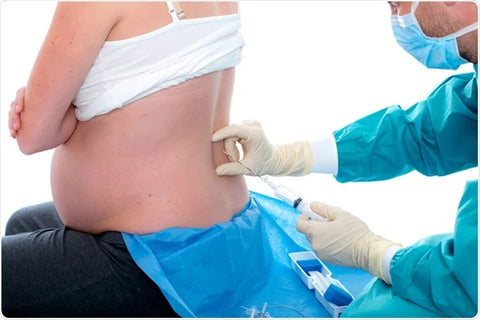
Epidural anesthesia involves an injection of a local anesthetic and an opioid into the lumbar epidural space, from which it gradually diffuses across the dura into the subarachnoid space. Here it acts primarily on the spinal nerve roots, and to a lesser degree on the spinal cord and paravertebral nerves.1 Since the epidural space is relatively larger than the spinal space, more anesthetic volume is required than with a spinal injection. The onset of action of an epidural is about 15 minutes; that of a spinal injection is almost instantaneous.
Ideally, epidural anesthesia results in segmental sympathetic and sensory nerve block and a decrease in endogenous catecholamines, thereby allowing the onset of pain relief.7 It can also cause hypotension or restoration of blood pressure (BP) to labor levels. While the degree of motor neuron effect depends upon the concentration of local anesthetic, most regional local anesthetics affect only skeletal muscle, not smooth muscle, at clinically relevant doses. This means that the amplitude or frequency of contractions in the myometrium is not diminished.8 The anesthetic is usually administered after the diagnosis of active labor has been established and the patient has requested pain relief.4 Most patients do not request an epidural before cervical dilation of 3 cm unless they are receiving oxytocin for labor augmentation. Recent data do not support findings that the use of an epidural block before cervical dilation of 5 cm will
adversely affect the subsequent course of labor.
Complications of Epidural Anesthesia
Perhaps the most common complication of epidural anesthesia is post dural puncture headache.4,5 It most frequently occurs in cases in which the dura is accidentally punctured, typically with a 17- or 18-gauge needle. This accidental puncturing, referred to as wet tap, occurs in about 1% of cases, and 70% of these patients develop post-dural puncture headaches. The headache usually results when leakage of cerebrospinal fluid leads to a reduction in intracranial pressure and compensatory cerebral vasodilation. In some patients, the headache is self-resolving; other patients may obtain relief by consuming caffeinated beverages. About 50% of patients can be definitively treated using an autologous epidural blood patch. In this procedure, a sterile injection of 15 to 25 mL of the patient’s blood is introduced into the epidural space, preferably at the site of the dural puncture, to produce a clot that blocks the meningeal leak. From 65% to 90% of patients obtain relief with this method. Epidural anesthesia has been identified as an independent risk factor for postpartum urinary
retention.13 This effect can be minimized by avoiding dense motor and sensory blocks. The use of epidural anesthesia increases the risk of vacuum- or forceps-assisted vaginal delivery.14 It also increases the duration of second-stage labor by 15 to 20 minutes and increases the need for oxytocin administration. Additionally, abnormal fetal heart tones during labor are seen in about 10% to 20% of patients with regional anesthesia, although this does not seem to adversely affect the neonate.
Administration of epidural anesthesia can cause hypertonic uterine contractions, possibly owing to a rapid increase in plasma epinephrine levels that leads to reduced beta-agonist tocolytic activity. This phenomenon, which may result from a very rapid onset of analgesia, can be reversed with the use of IV terbutaline 250 mcg, nitroglycerin 50 to 150 mcg, or sublingual nitroglycerin spray. 400 mcg.
About 80% of patients receiving epidural experience hypotension. Maternal BP may fall as a result of the elimination of painful stimuli and the onset of peripheral vasodilation. Although a modest decrease in BP may not have a significant effect, a large decrease may reduce uteroplacental blood flow and pose a threat to the fetus. For this reason, it is important to prevent, or promptly treat, significant hypotension. Administration of an isotonic electrolyte solution (e.g., lactated Ringer’s solution) before the epidural may prevent or reduce the extent of hypotension. Hypotension during epidural anesthesia may be treated with additional IV boluses of crystalloid solution and/or administration of small IV doses of a vasopressor, such as phenylephrine 50 to 100 mcg or ephedrine 5 to 10 mg.
Rare but serious complications of epidural anesthesia include neurologic injury, epidural hematoma, and deep epidural infection.5 Epidural hematoma and epidural abscess are seen in approximately 1 in 168,000 patients and 1 in 145,000 patients, respectively. Persistent neurologic injury is noted in 1 in 240,000 patients; transient neurologic injury is more common, occurring in
1 in 6,700.
High doses of local anesthetic injected intrathecally can cause a high spinal block, which presents as a respiratory compromise. Accidental high-dose IV injection can lead to seizures and cardiac arrest.1 Unintentional subarachnoid injection of local anesthetic can result in total spinal anesthesia.
To detect accidental subarachnoid or IV catheter placement, an epidural test dose is recommended. This typically involves the administration of 1.5% lidocaine 3 mL with 1:200,000 epinephrine.4 If the catheter has been placed intrathecally, spinal anesthesia is rapidly apparent, whereas IV placement is detected by an increase in heart rate of 20% or more.4 Studies have shown that epidural analgesia does not have a statistically significant impact on cesarean section risk, maternal satisfaction with pain relief, or long-term backache. Furthermore, epidural analgesia does not appear to have an immediate effect on neonatal status as determined by Apgar scores.
Contraindications to Epidural Anesthesia
Contraindications to any form of neuraxial anesthesia during labor include patient refusal, active maternal hemorrhage, increased intracranial pressure, septicemia, infection at or near the puncture site, and clinical signs of coagulopathy (including ongoing thromboprophylaxis with low-molecular-weight or unfractionated heparins). While the presence of an abnormal fetal heart- rate pattern is not a contraindication to epidural analgesia, many physicians prefer not to use epidural anesthesia in this situation. Inadequate training or experience on the part of those administering the anesthesia is also a contraindication.
Author: Dr. Iram Gill
Dr. Iram Gill is an MBBS doctor by profession and a Content Writer by passion. She is a mother as well and has observed the health-related challenges faced by mothers and babies. She wants to play her part in increasing access and support for breastfeeding and maternal health problems.